Medical reimbursements always look simple until you actually try to file one. You pay a doctor, buy medicines, maybe run a few tests, and naturally expect the money to come back smoothly. But this is where many people discover the reality.

Up To $5000 In Capital Health Claims why Documentation Matters because reimbursement decisions are not based on what you experienced, they are based on what you can prove. Most delayed or rejected claims happen for one reason: the paperwork didn’t clearly support the expense. Understanding Up To $5000 In Capital Health Claims Why Documentation Matters early saves you from repeated follow-ups, financial surprises, and frustration. Many policyholders think honesty alone is enough. After all, you were genuinely sick and genuinely treated. However, claim processors don’t know your situation personally. They rely entirely on records. Healthcare systems today operate through verification, not assumption. Every receipt, prescription, and report acts as a witness. If the documentation is unclear, the claim stops, even when the treatment was completely legitimate.
When a plan offers reimbursement within a fixed annual limit, each claim must be carefully validated. Administrators have to confirm that the expense was medically necessary and properly billed. This is exactly where Up To $5000 In Capital Health Claims Why Documentation Matters becomes practical. Your documents speak for you. A prescription links the illness to the treatment. A bill confirms the service was provided. A payment receipt shows the expense was actually paid. Without these records, even a genuine clinic visit can look like a personal purchase. Clear documentation protects you from rejection, speeds up processing, and reduces questions from reviewers.
Table of Contents
Up to $5000 in Capital Health Claims
| Key Information | Details |
|---|---|
| Annual Claim Limit | Up to $5000 eligible healthcare expenses |
| Eligible Treatments | Consultations, diagnostics, prescribed medicines, therapies |
| Required Proof | Prescription, itemized bill, reports, payment confirmation |
| Submission Window | Usually within 30–90 days |
| Processing Time | Around 7–30 working days |
| Common Rejection Reasons | Missing invoices, unclear prescription, late submission |
| Possible Review | Random audit or verification check |
Medical reimbursement is not complicated, but it is detail sensitive. The treatment may be genuine, but approval depends on proof. That is the central lesson behind Up To $5000 In Capital Health Claims Why Documentation Matters. The claim officer is not judging your illness; they are validating documentation. When paperwork is clear, reimbursement becomes routine. When records are missing, even legitimate expenses become doubtful. In practical terms, successful claims come down to organization. Keep records, submit early, and maintain consistency. Doing so ensures you actually receive the financial support the benefit is designed to provide.
Understanding The $5000 Claim Limit
- The yearly limit does not mean you automatically receive $5000. It simply represents the maximum amount you can be reimbursed within a policy year. Every individual expense must qualify on its own before it contributes to the total. For example, a consultation fee is reimbursed only when the practitioner is recognized and a diagnosis exists. A diagnostic test is covered only if a doctor recommended it. A medicine purchase is reimbursed only if it was prescribed.
- This is why Up To $5000 In Capital Health Claims Why Documentation Matters. The reimbursement total builds gradually from approved expenses, not from assumptions. A missing prescription can eliminate an entire bill from eligibility, even if the treatment was necessary. Many claimants discover this late in the year when they submit several months of medical bills together. Without proper documentation, a large portion of expenses becomes non-reimbursable.
What Documents Are Typically Required
Claims reviewers check three basic things: Was the treatment necessary? Did it happen? Was it paid? Each document answers one of these questions.
- Prescription: Shows the doctor evaluated a condition and recommended treatment.
- Itemized Bill: Breaks down services such as consultation, tests, or procedures. A single total amount is usually insufficient.
- Medical Reports: Diagnostic reports confirm the illness and support the treatment.
- Payment Proof: A stamped receipt, bank statement, or card slip verifies payment.
Together, these records form a chain of evidence. Remove one link and the claim weakens. That’s precisely why Up To $5000 In Capital Health Claims Why Documentation Matters in real situations.
Why Documentation Matters
Insurance administrators process thousands of claims every month. They cannot interview every patient or doctor. Documents become the only reliable source of verification.
Good documentation does three important things:
- First, it confirms medical necessity. A prescription connects the expense to a health condition.
- Second, it prevents fraud suspicion. Clear records demonstrate authenticity.
- Third, it speeds approval. Complete submissions reduce clarification requests.
A claim without documentation forces the reviewer to guess, and reviewers are not allowed to guess. They can only approve what is proven. That simple fact explains Up To $5000 In Capital Health Claims why Documentation Matters.
Common Documentation Mistakes
Many claims fail because of small avoidable errors.
- Unreadable Prescriptions: Handwritten notes without a stamp or registration number create doubt.
- Non-Itemized Bills: A receipt that only shows a total amount is often rejected.
- No Payment Confirmation: A bill alone does not prove the patient paid.
- Date Mismatch: If prescription and invoice dates differ widely, the claim appears questionable.
- Late Submission: Even a perfect claim may be declined if submitted after the allowed period.
Most people are surprised to learn that documentation mistakes cause more claim denials than policy limitations. Understanding Up To $5000 In Capital Health Claims Why Documentation Matters helps avoid these preventable issues.
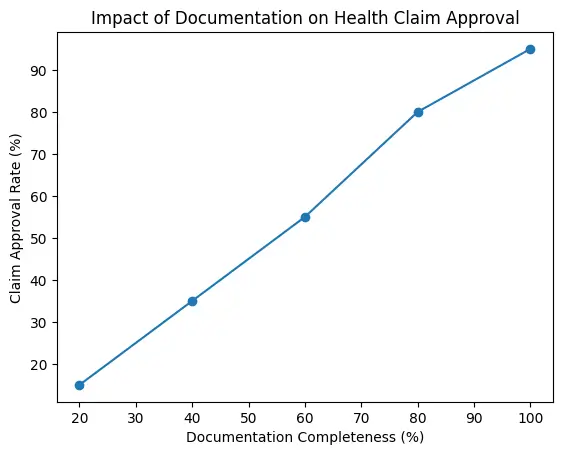
Step-By-Step Claim Process for Up to $5000 in Capital Health Settlement
Filing correctly is easier when you follow a routine.
- Visit a registered doctor
- Obtain written diagnosis and prescription
- Keep original invoices
- Collect diagnostic reports
- Fill the claim form carefully
- Attach payment proof and identification
- Submit before the deadline
This structured approach aligns perfectly with Up To $5000 In Capital Health Claims Why Documentation Matters because it eliminates missing information.
What Happens During a Review or Audit
- Sometimes a claim is flagged for additional verification. This does not mean rejection. It simply means the reviewer needs more assurance.
- A review may occur if the amount is unusually high, if several claims appear repetitive, or if the paperwork looks unclear. The administrator may contact the clinic or request additional proof.
- Claimants with organized records usually pass audits smoothly. Again, this demonstrates Up To $5000 In Capital Health Claims Why Documentation Matters beyond simple reimbursement it protects you during verification.
Tips To Maximize Reimbursement
A few habits can dramatically improve approval rates.
- Always request a stamped, itemized invoice before leaving the clinic.
- Take a photo of every document immediately. Paper can fade or get lost.
- Submit claims regularly instead of waiting until year-end.
- Keep prescriptions attached to the corresponding bills.
- Ensure the patient name matches policy records exactly.
FAQs on Up to $5000 in Capital Health Claims
1. What expenses usually qualify for reimbursement?
Doctor consultations, prescribed medicines, lab tests, and medically recommended therapies generally qualify when supported by proper documentation.
2. Why are claims rejected even when treatment is real?
Because the paperwork does not sufficiently prove medical necessity or payment verification.
3. How long does reimbursement normally take?
Processing typically takes between one and four weeks after verification.
4. Can digital copies be submitted?
Many systems accept scanned copies, but originals should always be preserved in case verification is required.